Illustration of the human intestine microbiome.
Findings might result in new choices for hypertensive sufferers who don’t reply to medicine.
Nearly half of the U.S. grownup inhabitants has hypertension — or hypertension — and about 20% of those sufferers have treatment-resistant hypertension. The explanation why some individuals are proof against therapy has been a thriller, however new research outcomes present that a sure intestine bacterium could also be an essential issue.
“Immediately, docs deal with resistant hypertension by including or substituting drugs, which may contribute to overdoses, extra unwanted side effects, and noncompliance,” stated Tao Yang, PhD, assistant professor on the College of Toledo. “A greater understanding of the connection between intestine microbes and drug efficacy might result in new therapy approaches for individuals who don’t reply to blood stress medicine. This might embrace new medication or modulating intestine microbiota with probiotics, antibiotics, and different strategies.”
By learning the intestine microbes of rats, Yang and colleagues found that a micro organism referred to as Coprococcus comes contributes to resistance to ACE inhibitors, one of many main drug courses used to deal with hypertension.
Yang will current the brand new analysis on the American Society for Pharmacology and Experimental Therapeutics annual assembly in the course of the Experimental Biology (EB) 2022 assembly, to be held on April 2-5, 2022, in Philadelphia.
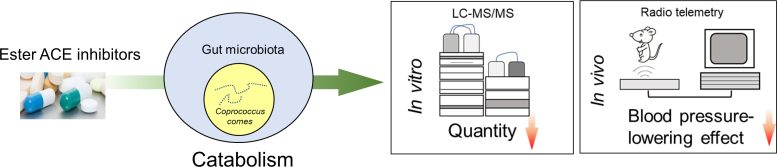
Researchers found that a bacterium referred to as Coprococcus comes could contribute to resistance to ACE inhibitors. They used research involving liquid chromatography–mass spectrometry and blood stress readings recorded by way of radio telemetry from a rat mannequin of hypertension. Credit score: Tao Yang, Division of Physiology and Pharmacology, College of Toledo
“Our final purpose is to discover a hyperlink between intestine microbial composition and enzymatic exercise and drug response effectiveness as a result of it will present a basis for making use of precision drugs to deal with resistant hypertension,” Yang stated.
Analysis has proven that the microorganisms in our intestine — collectively referred to as the intestine microbiota — comprise a wide range of enzymes that may have an effect on drug metabolism.
To seek out out if intestine microbiota would possibly play a task in resistance to blood stress drugs, Yang and colleagues administered a single dose of the ACE inhibitor quinapril to rats with hypertension. They discovered that quinapril was more practical at reducing blood stress in hypertensive rats with a decrease intestine microbiota load. Once they analyzed the composition of the intestine microbiota, C. comes emerged as an essential participant.
By means of extra experiments, the researchers discovered that C. comes can really break down quinapril. Additionally they noticed that giving C. comes and quinapril to hypertensive rats lowered blood stress lower than administering quinapril alone.
“We're nonetheless within the early phases of figuring out the interactions between intestine micro organism and antihypertensive drugs,” stated Yang. “Nevertheless, our present findings recommend that the identical drug might not be applicable for everybody as a result of every individual has a singular intestine microbial composition with a singular profile of enzymatic actions.”
The researchers at the moment are performing comparable experiments utilizing different kinds of intestine micro organism and extra blood stress drugs to additional discover how the intestine microbiota modulates the effectiveness of antihypertensive medication.
Tao Yang will current this analysis on from 10 a.m.–12 p.m., Tuesday, April 5, in Exhibit/Poster Corridor A-B, Pennsylvania Conference Middle (Poster Board Quantity B166) (summary). Contact the media staff for extra data or to acquire a free press cross to attend the assembly.
Assembly: Experimental Biology 2022
Post a Comment